Periodontal Dental Services
Prevention, Diagnosis, Treatment and Management of Periodontal Disease
Periodontal Disease Statistics
According to recent findings from the Centers for Disease Control and Prevention (CDC), half of Americans aged 30 or older have periodontitis, the more advanced form of periodontal disease. This equals approximately 64.7 million Americans.
The Prevalence of Periodontal Disease
Periodontal disease is the #1 cause of tooth loss among adults. Gum disease affects of 75% of adults at some point in their lives and of adults age 65-74, 26% have lost all of their teeth.
An Overview of Gum Disease
Periodontal disease is an inflammatory disease that affects the soft and hard structures that support the teeth. In its early stage, called gingivitis, the gums become swollen and red due to inflammation, which is the body’s natural response to the presence of harmful bacteria. In the more serious form of periodontal disease called periodontitis, the gums pull away from the tooth and supporting gum tissues are destroyed. Bone can be lost, and the teeth may loosen or eventually fall out.
The Symptoms of Gum Disease (Periodontitis)
The Causes of Gum Disease
The number one cause of gum disease is poor dental hygiene. Neglecting to brush and floss every day can allow plaque to build up and start the inflammation of the gingiva, or the gum around the base of your teeth.
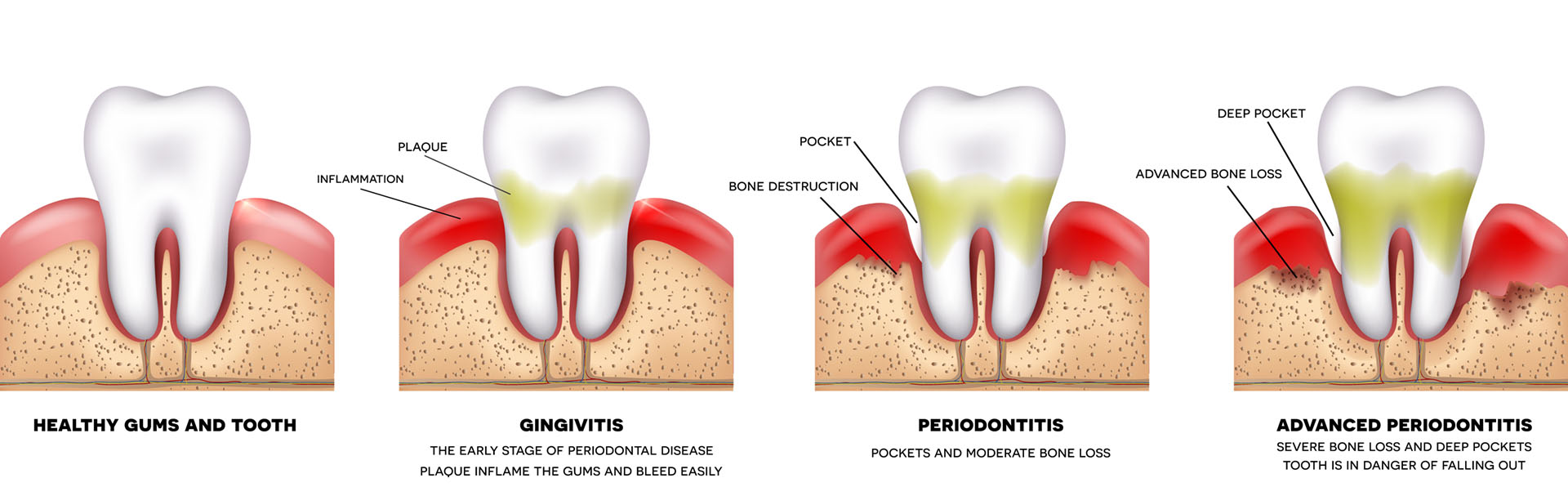
Chronic periodontitis, the most advanced form of the disease, progresses relatively slowly in most people, and is typically more evident in adulthood. Although inflammation as a result of a bacterial infection is behind all forms of periodontal disease, a variety of factors can influence the severity of the disease. Important risk factors include inherited or genetic susceptibility, smoking, lack of adequate home care, age, diet, health history, and medications.
Periodontal Disease is Connected To Your Overall Health
Several research studies have suggested that periodontal disease is connected to variety of other diseases, including heart disease, diabetes, and other systemic diseases. Scientists believe that inflammation may be the basis for the link between these systemic diseases. While periodontists are experts in treating oral inflammation, additional research is needed to better understand how treating periodontal disease may reduce the risk of developing other inflammatory diseases.
Diagnosing Periodontal Disease
Dr. Glaser and your hygienists typically rely on a visual assessment of the patient’s overall oral condition, charting pocket depths with a periodontal probe, and their dental health history. This visual/mechanical method of assessing periodontal disease status can only tell whether or not disease is present. There are other tests currently available that go beyond basic and subjective visual assessment to provide dental professionals with the detailed genetic and biological information required to better determine the appropriate treatment regimen for each individual patient. This information includes evaluating the inflammatory burden that is causing periodontal disease, as well as looking at the patient’s unique genetic susceptibility to periodontal disease.
Non-Surgical Periodontal Treatment
The American Academy of Periodontology treatment guidelines stress that periodontal health should be achieved in the least invasive and most cost-effective manner. This is often accomplished through non-surgical treatment.
Non-Surgical Periodontal maintenance is the ongoing treatment for patients who have periodontitis, which is a chronic and non-curable bacterial infection. The objective of periodontal maintenance is to keep the disease under control. Scaling and root planing or surgical periodontal procedures are ineffective in the long term without an effective periodontal maintenance regimen
Glaser Dental offers a wide range of non-surgical treatments which, in many cases, can eliminate the need for painful surgery:
- Seeing your hygienist every 3-4 months for removal of plaque & calculus below the gum line (see scaling & root planing below)
- Maintaining your prescribed home care that could include a medicated rinse, oral prescriptions, and of course flossing and brushing
- Smoking secession
The rationale for three-month maintenance intervals is not arbitrary; it is based on a sound bacterial rationale. Biofilm re-colinization will occur in three to 12 weeks from its disruption.
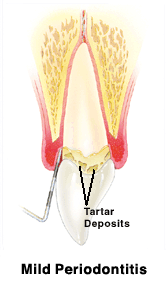
Scaling & Root Planing (SRP)Patients diagnosed with active periodontal disease cannot benefit from a healthy mouth cleaning because they require treatment above and below the gum line. These patients generally receive Scaling & Root Planing, a non-surgical treatment that removes plaque and calculus [tartar] and smooths out exposed the tooth root to remove bacterial toxins. Scaling and root planing is often followed by adjunctive therapy such as local delivery antimicrobials as needed on a case-by-case basis. Treatment may be limited to one time but typically is performed in phases in multiple visits. Treatment may include:
Surgical Periodontal Treatment
If the patient ignores, or refuses treatment early on, the disease may progress to a point where surgical treatment may be the only option to save the tooth/teeth. That is when a periodontist would play a role in patient care. They surgically cut the gums and clean out the disease. Dr. Glaser will refer you to a periodontist for treatment.
Periodontal Pocket Reduction Procedures
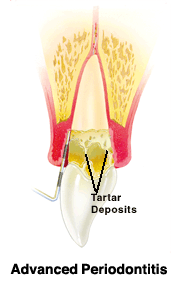
Your bone and gum tissue should fit snugly around your teeth like a turtleneck fits around your neck. When you have periodontal disease, this supporting tissue and bone is destroyed, forming “pockets” around the teeth.
Over time, these pockets become deeper, providing a larger space for bacteria to live. As bacteria develop around the teeth, they can accumulate and advance under the gum tissue. These deep pockets collect even more bacteria, resulting in further bone and tissue loss. Eventually, if too much bone is lost, the teeth will need to be extracted.
Your periodontist has measured the depth of your pocket(s). A periodontal pocket reduction procedure has been recommended because you have pockets that are too deep to clean with daily at-home oral hygiene and a professional care routine.
During this procedure, your periodontist folds back the gum tissue and removes the disease-causing bacteria before securing the tissue into place. In some cases, irregular surfaces of the damaged bone are smoothed to limit areas where disease-causing bacteria can hide. This allows the gum tissue to better reattach to healthy bone.
Reducing pocket depth and eliminating existing bacteria are important to prevent damage caused by the progression of periodontal disease and to help you maintain a healthy smile. Eliminating bacteria alone may not be sufficient to prevent disease recurrence. Deeper pockets are more difficult for you and your dental care professional to clean, so it’s important for you to reduce them. Reduced pockets and a combination of daily oral hygiene and professional maintenance care increase your chances of keeping your natural teeth – and decrease the chance of serious health problems associated with periodontal disease.
Managing Your Periodontal Disease
After a deep cleaning to remove most of the bacteria that is damaging your gums, Dr. Glaser may also give you a medicated mouth rinse, like Chlorhexidine, to use at home. Your treatment will depend on the seriousness of your gum disease and how you’ve responed to previous treatments. Dr. Glaser will develop a personalized treatment plan to address your specific case.
What can you do to stay healthy?
Gum disease can usually be treated successfully. If you have gum disease, here are some suggestions to help keep your gums healthy:
- Get regular cleanings every 3-4 months. This is not an arbitrary timeline but based on bio-film re-colinization will occur in 3-12 weeks from its disruption. This step is imperative to keeping destructive bacteria under control.
- Floss your teeth daily
- Brush twice a day with a soft-bristled toothbrush and fluoride toothpaste
- Visit your dentist at least every six months for oral exams and cleanings
- Use any at-home products Dr. Glaser recommends such as Chlorhexidine mouthrinse or prescription fluoride toothpaste
- Do not chew or smoke tobacco
The bottom line is that the regular and effective removal of dental plaque is the key to achieving and maintaining your oral health!